What Are the Signs That a Hospital Mattress Needs to Be Replaced Immediately?
In any care home or healthcare facility, a hospital mattress is far more than a piece of furniture — it is a frontline tool in patient care. It supports healing, prevents pressure injuries, and directly impacts the comfort and dignity of patients who spend many hours each day in bed.
Yet despite this critical role, mattress replacement is one of the most overlooked aspects of care home maintenance in Ireland. Many facilities wait until a mattress is visibly ruined before acting — by which point the damage to patient care may already be done.
So how do you know when a hospital mattress needs to go — not next month, but right now? This guide breaks down the key warning signs that demand immediate action.
Why timely replacement matters
A deteriorating hospital mattress doesn't just cause discomfort. It can contribute to pressure ulcers, poor sleep quality, increased infection risk, and a decline in the overall standard of care. For bedridden or high-dependency patients, the stakes are especially high.
Care homes in Ireland are increasingly under regulatory scrutiny when it comes to the quality of patient environments. A proactive approach to mattress replacement is not just best practice — it is a care obligation.
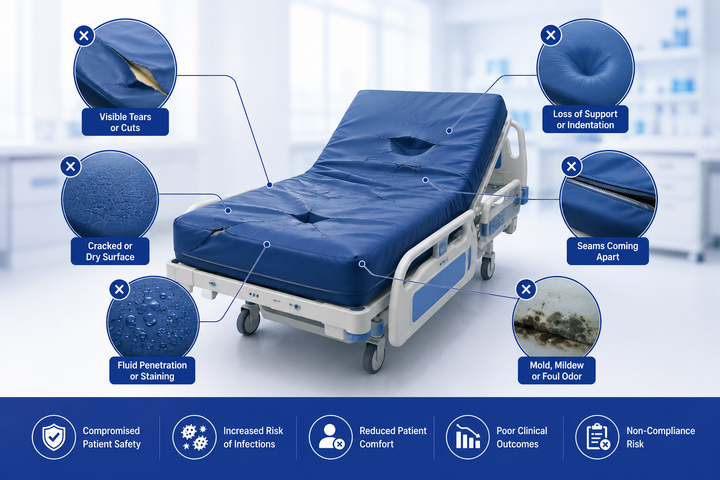
The 7 signs a hospital mattress needs immediate replacement
Important: In a care home setting, even one of the above signs is sufficient reason to begin the replacement process. You do not need multiple indicators — acting early protects both patients and your facility's compliance standards.
Common mistakes care homes make
Despite the clear signs listed above, many care facilities fall into predictable traps when managing hospital mattresses:
- Waiting for a mattress to be completely unusable before replacing it
- Relying on visual inspection alone without assessing functional performance
- Using the same mattress type across all patients regardless of individual care needs
- Delaying replacement due to budget cycles rather than clinical need
- Failing to maintain inspection records that could flag deteriorating stock early
These gaps, often unintentional, can quietly undermine the standard of care being delivered — and may expose facilities to regulatory risk during HIQA inspections.
What to do when you spot the signs
Once a warning sign is identified, the process should be straightforward:
- Remove the mattress from use immediately if there is any hygiene or structural concern
- Document the reason for replacement as part of your facility's maintenance log
- Assess the individual patient's needs before selecting a replacement — not all mattresses are appropriate for all patients
- Contact a reliable healthcare supplier to ensure quick and consistent restocking
- Review your wider mattress inventory to check if others are approaching the end of their useful life
The most effective care homes do not wait for signs of failure — they build systems that prevent failure from becoming a problem in the first place. This means scheduling routine inspections, setting clear replacement timelines based on mattress type and usage, and empowering care staff to flag concerns without delay.
A scheduled replacement cycle, even a simple one, ensures that mattresses are never quietly past their useful life without anyone noticing. It also makes budgeting more predictable and reduces the likelihood of reactive, emergency replacements that can disrupt care continuity.
Conclusion
Recognising when a hospital mattress needs immediate replacement is one of the simplest and most impactful steps a care home can take to protect its patients. From visible damage and persistent odours to loss of pressure-relief function and expired lifespans, the signs are often clear — if you know what to look for.
The key is to act early, document consistently, and partner with a supplier who understands the specific demands of Irish care home environments. Medguard Healthcare supports care providers across Ireland with a comprehensive range of hospital mattresses designed to meet clinical needs, hygiene standards, and the comfort of long-term patients — making it easier for facilities to maintain quality care at every stage of the mattress lifecycle.